Monkeypox usually self-limiting but may be severe in some individuals: WHO
Published :
Updated :

Monkeypox is usually self-limiting but may be severe in some individuals, such as children, pregnant women or persons with immune suppression due to other health conditions, says the World Health Organization (WHO) on Sunday, reports UNB.
Eating inadequately cooked meat and other animal products of infected animals is a possible risk factor, according to the WHO which is dedicated to the well-being of all people and guided by science.
Monkeypox virus is transmitted from one person to another by close contact with lesions, body fluids, respiratory droplets and contaminated materials such as bedding. The incubation period of monkeypox is usually from 6 to 13 days but can range from 5 to 21 days.
As of now, 92 laboratory confirmed cases, and 28 suspected cases of monkeypox with investigations ongoing, have been reported to the WHO from 12 Member States that are not endemic for monkeypox virus.
Monkeypox endemic countries are Benin, Cameroon, the Central African Republic, the Democratic Republic of the Congo, Gabon, Ghana (identified in animals only), Ivory Coast, Liberia, Nigeria, the Republic of the Congo, Sierra Leone, and South Sudan.
Since 13 May 2022, cases of monkeypox have been reported to WHO from 12 Member States that are not endemic for monkeypox virus, across three WHO regions.
Epidemiological investigations are ongoing, however, reported cases thus far have no established travel links to endemic areas.
The situation is evolving and WHO expects there will be more cases of monkeypox identified as surveillance expands in non-endemic countries.
Reported cases thus far have no established travel links to an endemic area, said the WHO on Sunday.
Based on currently available information, cases have mainly but not exclusively been identified amongst men who have sex with men (MSM) seeking care in primary care and sexual health clinics.
To date, all cases whose samples were confirmed by PCR have been identified as being infected with the West African clade.
Genome sequence from a swab sample from a confirmed case in Portugal, indicated a close match of the monkeypox virus causing the current outbreak, to exported cases from Nigeria to the United Kingdom, Israel and Singapore in 2018 and 2019.
The identification of confirmed and suspected cases of monkeypox with no direct travel links to an endemic area represents a highly unusual event.
Surveillance to date in non-endemic areas has been limited, but is now expanding.
WHO expects that more cases in non-endemic areas are likely to be reported. Available information suggests that human-to-human transmission is occurring among people in close physical contact with cases who are symptomatic.
In addition to this new outbreak, WHO continues to receive updates on the status of ongoing reports of monkeypox cases through established surveillance mechanisms (Integrated Disease Surveillance and Response) for cases in endemic countries [1], as summarized in table 2.
Epidemiology of the Disease
Monkeypox is a viral zoonosis (a virus transmitted to humans from animals) with symptoms very similar to those seen in the past in smallpox patients, although it is clinically less severe.
It is caused by the monkeypox virus which belongs to the orthopoxvirus genus of the Poxviridae family.
There are two clades of monkeypox virus: the West African clade and the Congo Basin (Central African) clade.
The name monkeypox originates from the initial discovery of the virus in monkeys in a Danish laboratory in 1958. The first human case was identified in a child in the Democratic Republic of the Congo in 1970.
Various animal species have been identified as susceptible to the monkeypox virus. Uncertainty remains on the natural history of the monkeypox virus and further studies are needed to identify the exact reservoir(s) and how virus circulation is maintained in nature.
Human infections with the West African clade appear to cause less severe disease compared to the Congo Basin clade, with a case fatality rate of 3.6% compared to 10.6% for the Congo Basin clade.
Suspected Case Symptoms
A person of any age presenting in a monkeypox non-endemic country with an unexplained acute rash; and one or more of the following signs or symptoms, since 15 March 2022 – headache, acute onset of fever (>38.5oC), lymphadenopathy (swollen lymph nodes), myalgia (muscle and body aches), back pain and asthenia (profound weakness).
WHO Risk Assessment
Endemic monkeypox disease is normally geographically limited to West and Central Africa.
The identification of confirmed and suspected cases of monkeypox without any travel history to an endemic area in multiple countries is atypical, hence, there is an urgent need to raise awareness about monkeypox and undertake comprehensive case finding and isolation (provided with supportive care), contact tracing and supportive care to limit further onward transmission.
Cross-protective immunity from smallpox vaccination will be limited to older persons, since populations worldwide under the age of 40 or 50 years no longer benefit from the protection afforded by prior smallpox vaccination programmes.
There is little immunity to monkeypox among younger people living in non-endemic countries since the virus has not been present there.
WHO Advice
Identification of additional cases and further onward spread in the countries currently reporting cases and other Member States is likely.
Any patient with suspected monkeypox should be investigated and if confirmed, isolated until their lesions have crusted, the scab has fallen off and a fresh layer of skin has formed underneath.
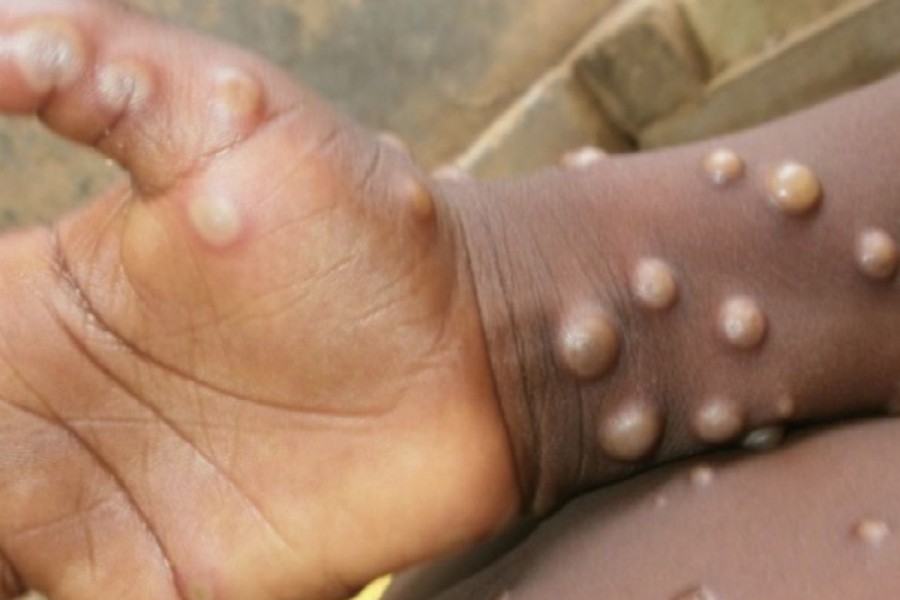
Countries should be on the alert for signals related to patients presenting with an atypical rash that progresses in sequential stages – macules, papules, vesicles, pustules, scabs, at the same stage of development over all affected areas of the body – that may be associated with fever, enlarged lymph nodes, back pain, and muscle aches.
In non-endemic countries, one case is considered an outbreak. Because of the public health risks associated with a single case of monkeypox, clinicians should report suspected cases immediately to national or local public health authorities regardless of whether they are also exploring other potential diagnoses.


 For all latest news, follow The Financial Express Google News channel.
For all latest news, follow The Financial Express Google News channel.